Senior Consultant Neurosurgeon & Endoscopic Spine Surgeon
Apollo Hospitals, Secunderabad, Hyderabad
17+ years experience · 7,500+ surgeries · Minimally invasive spine & pituitary surgery

Signature Procedures
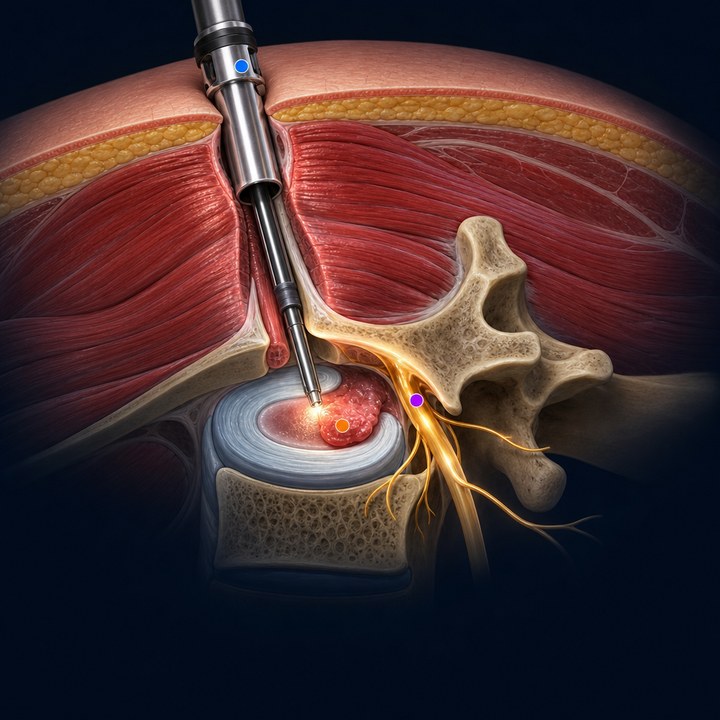
Endoscopic Spine Surgery
Keyhole monoportal disc surgery through an 8 mm incision — muscle-sparing, most patients walk the same day.
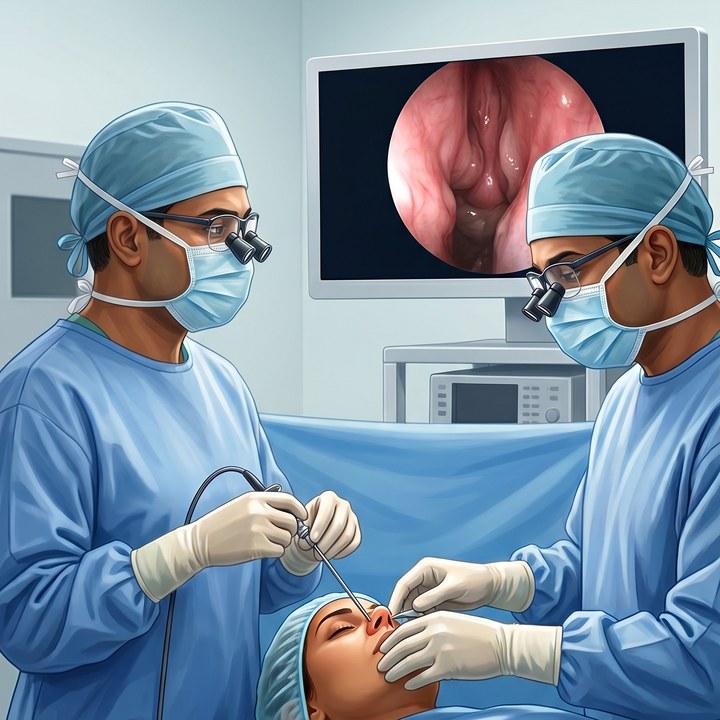
Pituitary Tumour Surgery
Scarless transnasal endoscopic removal — through the nose, no skull cut, with a combined neurosurgery & ENT team.
Skull Base Surgery
Complex skull base tumours treated by a dual neurosurgeon + ENT team — a rare combined expertise in Hyderabad.
Why Patients Choose Dr. Kalyan
- A neurosurgeon operating on the spine — nerve expertise, not just bone expertise
- 17+ years and 7,500+ brain & spine surgeries
- Minimally invasive, muscle-sparing endoscopic techniques — faster recovery
- Functional Dynamic EMG rehabilitation for a stronger, lasting recovery
- 196+ patient-education videos on YouTube, in plain language
- 4 consultation locations across Hyderabad, anchored at Apollo Secunderabad
Talk to Dr. Kalyan’s Team
WhatsApp your MRI scans or questions to 85200 03683 — the team typically responds within a few hours during working hours. Consultations at Apollo Hospitals, Secunderabad.
